DENVER — While there is no dispute that the coronavirus pandemic has yet to hit its peak, data predicting when that will happen, and the number of people that will be infected, hospitalized and die continues to vary vastly at the state and national level.
Last week, White House coronavirus task force member Dr. Deborah Birx, announced that the data being disseminated does not match the actual data coming in as the pandemic enters its second month after the first official active cases in the U.S. were announced.
Birx is a world-renowned medical expert, with a decades-long career in immunology, infectious disease, research and global health. She was appointed to lead the federal government response to COVID-19 as the Coronavirus Response Coordinator.
At a press briefing last week, information given by Birx contradicted information Colorado Governor Jared Polis continues to cite, as recently as Monday.
At Polis’ press briefing on Monday, University of Colorado School of Medicine Dr. Marc Moss explained the shortage of needed medical equipment and how he and other doctors are trying to find an ethical solution to making decisions about life saving measures should hospitals’ fears of the shortage come to pass when the cases peak.
Birx said that is not what the American people should be focused on.
“It’s our job collectively to assure the American people,” she said, adding people do not need to unnecessarily debate advanced medical directives, such as do not resuscitate orders.
“Please for the reassurance of people around the world, there is no situation in the United States right now that warrants that kind of discussion,” she said. “To say that to the American people, to make the implication that when they need a hospital bed it’s not going to be there, or when they need that ventilator, it’s not going to be there, we don’t have evidence of that.”
2018 ICU Total and Licensed Beds by Sherrie A Peif on Scribd
In Colorado, Polis cites data that reports there are 1,849 total Intensive Care Unit and Critical Care Unit beds and 22,851 regular hospital beds. However, that data, which was requested by Complete Colorado, is from a 2018 Medicare cost reports, a required filing for all hospitals.
Cara Welch, the director of communications for the Colorado Hospital Association said the bed count has changed since that report.
“It’s two years old already and should be seen as a baseline, not current,” Welch said “We know that many of our hospitals and health systems had added capacity in those two years, and many continue to add beds in this current environment because of the surge that we are anticipating.”
Kelly Tracer, media relations specialist for UCHealth, confirmed that is the case at UC hospitals in Northern Colorado.
According to the 2018 report, Medical Center of the Rockies in Loveland has 174 beds. Tracer reports that number now at 187. Likewise, Poudre Valley Hospital in Fort Collins is listed at 255 beds, that number is now 296. And the UCHealth Greeley Hospital did not exist at the time of the report, so an additional 50 beds are now located there.
Tracer did not comment on ICU beds because she said that number changes constantly.
“UCHealth is proactively managing our capacity and freeing up inpatient beds when possible to make sure we’re ready to handle larger numbers of patients should this be needed,” Tracer said. “We are currently experiencing fewer patients overall, particularly in our emergency departments, but this was part of the strategy we put in place to make sure that we could handle an influx of very sick patients who would require critical care. This strategy included postponing any elective procedures or surgeries.”
DIFFERENT DATA SETS —
Birx said the original coronavirus model is no longer valid. It was created by epidemiologist Neil Ferguson, who initially said the number of deaths in the U.K. would be close to 500,000 and 2.2 million in the United States. Ferguson recently adjusted the U.K. numbers to 20,000.
“Half a million to 20,000,” she said. “We are looking into this in great detail to understand that adjustment. … You have to have a large group of people who are a-symptomatic — who never presented for any test in order to have the kind of numbers that were predicted.”
Birx said that in no country to date — with very few exceptions of very low populated countries — have officials seen an attack rate over 1 in 1,000. They are working hard to get an antibody test to figure out who all the people are that are supposed to be infected with it, or if they even exist, she said.
“So either we’re only measuring the tip of iceberg and symptomatic cases and underneath it are a large group of people … or we had the transmission completely wrong,” Birx said, adding the predictions of the early model don’t match the reality on the ground in China, South Korea or Italy.
“We are about five times the size of Italy,” she said. “If we were Italy and did all those divisions, Italy should have close to 400,000 deaths. They are not close to achieving that.”
Birx scaled back the death toll from 2.2 million to 200,000, after creating a new model based on information coming from states across the U.S. She reminded everyone that “models are models.”
“There is enough real experience now with the coronavirus on the ground to really make these predictions much, more sound,” Birx said. “There is no model right now — no reality on the ground where we can see that 60 to 70 percent of Americans are going to get infected in the next eight to 12 weeks. I just want to be clear about that.”
Birx added the Centers for Disease Control (CDC) and others under her are adapting to the reality on the ground and looking very carefully at the models and learning clearly from South Korea, Italy and Spain.
Birx’s comments and the data her group is using are in contrast to those still being used by Governor Jared Polis, who says the number of deaths in Colorado alone could reach more than 11,000 people by June 1, even if 60 percent of residents practice social distancing.
By comparison, the model touted by Birx, predicts slightly more than 2,000 by August.
Polis gave a “data conference” last week after a story in the Colorado Sun questioned the data being used to shut down much of the economy in an effort to slow the progress of the infection.
According to the Colorado Sun, the model being used by Polis is one built by Kathryn Colborn, an associate professor in the Department of Surgery on the University of Colorado’s Anschutz medical Campus. Colborn also has a background in infectious disease statistics, the Sun reported.
Part of the problem with Polis’ data, some say, is the Colorado Department of Public Health and Environment (CDPHE) is now reporting total positive cases to include both actual tests for the virus and “guesses” by medical professionals based on the symptoms presented and the likelihood the patient was exposed.
Symptoms of the virus include fever, cough and shortness of breath, symptoms that can also present with influenza, bronchitis, the common cold or many other illnesses that are common this time of year.
Along with the numbers reported each day by the CDPHE, Colborn uses two additional pieces of information, the Sun reported. The Ro or “R naught,” an estimate of how many people a single infected person can infect, is usually obtained by the examination of large amounts of data from the relevant population.
The Ro used in this analysis is not necessarily typical of those found by other researchers, including the Institute for Health Metrics and Evaluation (IHME) at the University of Washington, which is the model touted by Birx. Birx said at a recent press briefing that the IHME model is producing the same numbers as the model she created to advise the CDC.
Colborn confirmed to the Sun that the numbers are an estimate using a formula developed in England and based on the percentage of patients hospitalized with COVID-19. That guesswork arrived at a number somewhere between 3,000 and 4,000 at a time when the state was officially reporting just under 1,500.
The other data point Colborn uses is how many total people are known to be currently infected. But that the CDPHE is also reporting estimates of the infected only compounds the speculation, said Dr. Dave Kisker, a Johnstown resident with a long career in data modeling.
“Unlike the IHME model, the Polis model appears to be largely guesswork, using Ro estimates that are far outside the normal range of 1.5-2.5, and are not based on Colorado results, but apparently on results from other countries,” Kisker said. “While dealing with incomplete data is certainly challenging, it’s critically important that the applicability of a model of such data be understood.”
Kisker has degrees in chemistry, applied physics and a Ph.D. from Stanford University in the study of electronic materials. During his career, he has routinely modeled many complex physical systems.
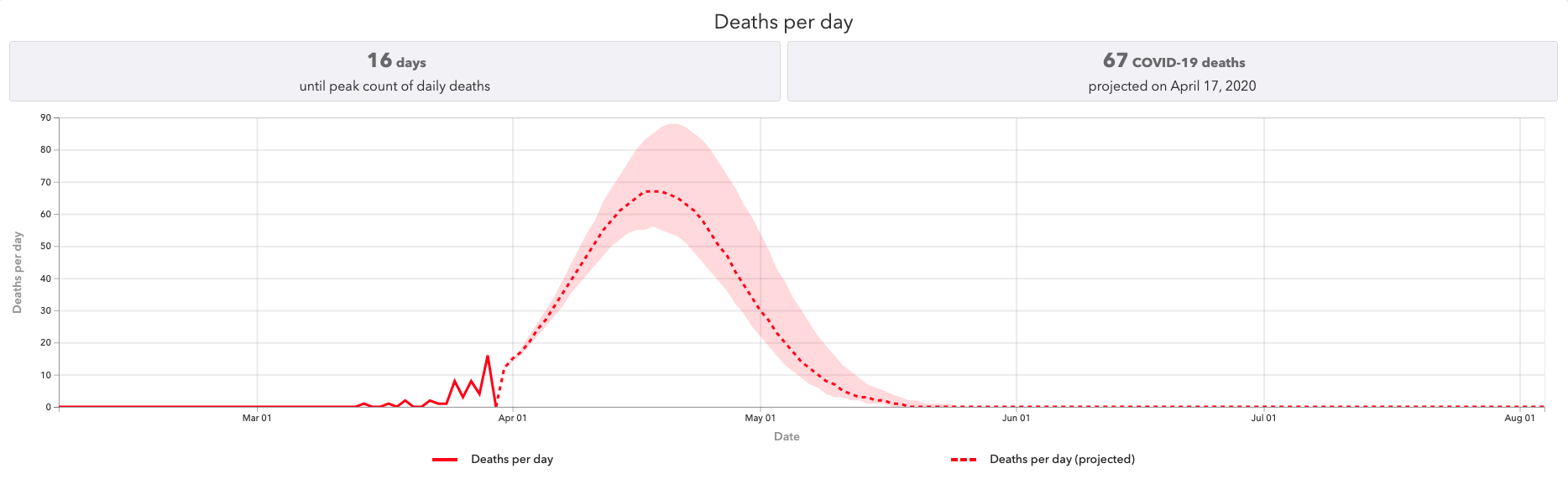
The IHME model, which does take into consideration when Polis put in place the current “stay at home” order (March 26), when he closed educational facilities (March 23) and when he closed non-essential services (March 26), predicts April 17 to be the peak date for the virus to hit the state. As of April 1, IHME predicts that on April 17 Colorado Hospitals will need 6,776 beds, 1,032 ICU beds and 826 ventilators. It predicts a per-day peak of 67 deaths by that point, with a total death count of 1,683 deaths by Aug. 4. The data is continually changing.
Polis on Monday said that while closing restaurants and bars has slowed the spread, it won’t be known for two more weeks whether his model’s prediction of 11,000 deaths by June will be impacted by his full stay at home order and a 60 percent social distancing compliance rate.


